 Overview & Introduction
Overview & Introduction
Feelings About Breast Cancer
Partnering with Your Healthcare Provider
When You Start Treatment
Sample Questions
General Questions
Sample Comparision Table
Complementary and Integrative Treatments
After Treatment and Ongoing Treatments
Let’s Not Forget the Caregivers
Turning Anger into Action
If you’re reading this packet it probably means you or someone you care about has recently been diagnosed with breast cancer. Breast cancer is both all too common and incredibly individual. Each year, nearly a quarter of a million women are diagnosed with breast cancer. Yet no two people have the same experience. And there isn’t a roadmap that works for everyone.
This resource is intended to help you make deeply personal treatment decisions based on current information about breast cancer. It should be paired with Breast Cancer Action’s What You Need to Know About Breast Cancer overview, which provides information about the various types of breast cancer and range of possible treatments.
Most people diagnosed with breast cancer face several treatment options, each with its own benefits and potential harms. These isn’t a “right” choice that’s best for everyone and it’s up to each of us to figure out what is right for us. Sometimes, doing nothing is a reasonable option and should be considered and weighed against possible interventions. We may not be able to control if we get breast cancer, but we each get to make our own decisions about tests, treatments, and care within the range of options for our specific diagnosis.
That said, it can feel overwhelming to be presented with all these choices! You may feel that you don’t know where to begin or even what questions to ask. There are so many impenetrable medical terms to learn, so many options to consider, so many feelings to juggle. Few of us are experts on breast cancer when we are diagnosed, and for many of us this is the first serious diagnosis we have ever faced.
We want you to know you are not alone and those who have been down this road before you have a good deal of wisdom to share to help you navigate the information, advocate for yourself, and get the care that works best for you. This document was written with input from others who have gone through this experience. Breast Cancer Action brings a patient perspective to the data, and you can rest assured that since we never take funding from pharmaceutical or biotechnology companies, we are not beholden to any one treatment, drug, or company.
Our hope is that the information, ideas, and tips gathered here will make living with your breast cancer diagnosis easier for you and your loved ones. And most importantly, we hope we can support you so you can make the right decisions for you.
Being diagnosed with breast cancer can stir up a lot of powerful feelings. Many of us are scared when we are first diagnosed: we didn’t know what it all means and we are afraid of the unknown, possible pain, physical changes, unwanted side effects, and even death. Practical questions about treatment, financial costs, personal relationships, and quality of life can make us feel anxious. It is easy to feel lost and overwhelmed by unfamiliar medical terms, procedures, and advice. Some of us feel angry, whether at the unfairness of getting cancer or the insensitivity of people who just don’t “get it.” We may feel frustrated at the bureaucratic hassles on top of everything else. Whatever you are feeling is perfectly normal. There is no single right way to feel or best way to handle a breast cancer diagnosis. And your feelings will probably change over time.
Very few, if any, of the decisions we face as part of a diagnosis are cut and dry, and all of the data has to be weighed according to our individual preferences, circumstances, and values. Even though it can feel like there’s a mythical “average” patient who is the subject of a lot of the resources out there, many of you reading this may be younger or older than average, you may not identify as a woman, or you may have complex health issues unrelated to breast cancer. There isn’t one way to experience breast cancer; and the most important thing you can do is to find the information and support you need to figure out the way that is best for you.

The truth is that, when we’re first diagnosed, there is no way to know exactly what is going to happen in our individual case. We each make the best decisions we can, based on the information that is available to us at the time. For this reason, we encourage you to take the time you need to talk to healthcare workers and others who have personal experience with breast cancer so you can ask questions, and consider multiple viewpoints and options. It’s important you feel comfortable with whatever decisions you make.
Over the years we have gathered some basic and not-so-basic suggestions that have been helpful to those who have just received a breast cancer diagnosis. We’ve grouped these suggestions under headings to give them some context. No matter where you are in the process, you may find some of these tips helpful.
 For some health conditions, there is a single treatment that is the clear standard of care, and patient preference has a limited role (for example whether a broken bone requires a cast or surgery.) With breast cancer, however, there is often more than one reasonable path forward, each with possible benefits, limitations, and harms.
For some health conditions, there is a single treatment that is the clear standard of care, and patient preference has a limited role (for example whether a broken bone requires a cast or surgery.) With breast cancer, however, there is often more than one reasonable path forward, each with possible benefits, limitations, and harms.
Make sure your healthcare provider explains your treatment options so they are understandable to you. Clearly and patiently answering all of your questions is an essential part of their job—so don’t be shy and don’t hold back. The provider’s medical expertise is important for understanding your treatment options, including risks and benefits, but only you know all the relevant factors about what this will mean for you, including how it fits with your own preferences and values. Most healthcare providers appreciate this time with patients and feel that their job is not only to treat you but to support your informed decision-making, based on your individual circumstances, values, and preferences.
Ask for and accept help. We know it can sometimes be hard to ask for and accept help. And not all of us have a big, local support network that can step up. We’ve found that support can come from many places besides family and close friends who live nearby. Many of us have been surprised and deeply touched by support we’ve gotten from acquaintances who are not yet good friends, individual healthcare providers (often nurses), support groups, online communities, and other places. Consider reaching out if you need help or support that you aren’t currently getting.
For free, one-on-one breast cancer information and resources, reach out:
• phone: 800/877.2.STOPBC
• email: info@bcaction.org
Being diagnosed with breast cancer may feel like taking a crash course in biology and medicine. Few of us come to this with existing knowledge about breast cancer. There is a lot of new information and a lot to learn. Most importantly, you want to know what your diagnosis means for you.
Medicine involves uncertainty and there is no way to know exactly what will happen in your specific case. Your providers will talk about likelihood, probabilities, percentages, and overall statistics. When discussing treatment options, it is important to understand the difference between the relative benefit (or risk) and the absolute benefit (or risk).
Here are some sample questions that may be helpful to get you started as you discuss your diagnosis and your treatment options with your healthcare provider. Not all of these questions may feel important to you. It may be helpful to rewrite the questions in your own words and add your own questions.
Often the answers to one question will spark new questions. This is a conversation with your healthcare provider, and you deserve the time and attention you need to have all of your questions answered to your satisfaction.
Some people are diagnosed with advanced or metastatic cancer when they are first diagnosed. We want you to know that, while this is less common than an early-stage diagnosis, you are not alone. If it’s possible for you, we recommend you seek treatment (or at least a second opinion) from a major cancer/teaching hospital. Major cancer centers see more people who have advanced cancers and are likely to have access to and involvement with the latest treatments, as well as access to new or emerging treatments and trials. And because you may be in treatment for some time, it’s even more important to see your medical provider as a trusted ally, someone you can speak honestly with and who can be your partner in decision-making. Questions to add to your list:
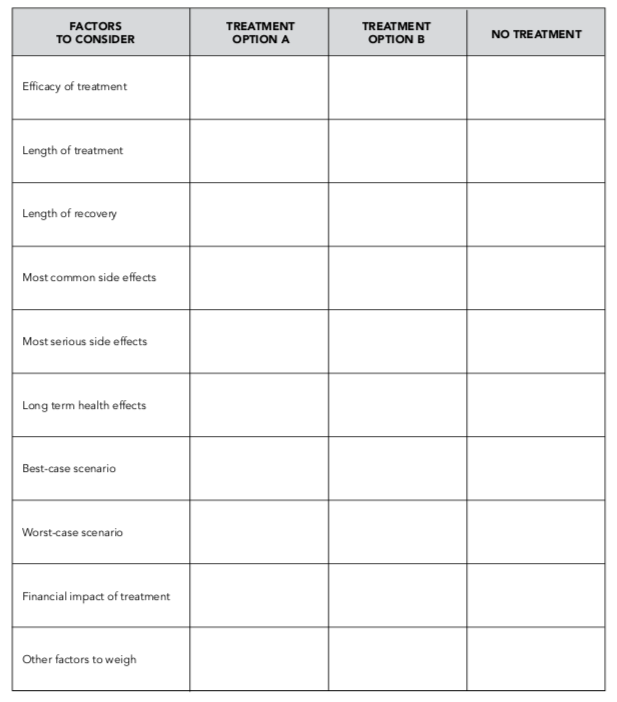
Some people find it useful to make a table to compare treatment options side-by-side, like the example below. As you learn about your specific options, you may want to customize the chart to add other factors that are important to you.
Many people are concerned about the side effects of conventional cancer treatments and decided to look into non-Western healthcare. It is estimated that nearly a third of Americans use nonconventional medicine. These treatments may include supplements (such as vitamins, herbs, and probiotics), mind-body techniques, or non-Western healthcare (such as acupuncture, Ayurvedic medicine, or naturopathy).
The terms “alternative,” “complementary,” and “integrative” are sometimes used interchangeably, but they have distinct meanings. Alternative therapy is rare and is used in place of any conventional medical treatment. Complementary therapies are used alongside conventional Western medicine and are sometimes seen as a tool to support the body during treatment. Integrative healthcare brings together conventional and complementary approaches in a coordinated way. More and more cancer centers are adding integrative approaches to their programs.
Conventional cancer treatments, such as chemotherapy, are approved by the U.S. Food and Drug Administration (FDA) after rigorous testing through clinical trials to prove they work and to evaluate the side effects and risks of treatment. These trials take time and are expensive; the result is that medical research usually focuses on treatments that can be patented and make a lot of money.

Most nonconventional treatments cannot be patented and have not been through such rigorous testing, although there have been some limited clinical trials of acupuncture and some supplements. This leaves patients in a difficult situation because the lack of data does not mean that these treatments are necessarily ineffective, but there isn’t proof that the treatment works, or how it may interact with conventional treatments. There also isn’t data about the harms, side effects, or most effective dosing. Remember that the fact that alternative treatments are considered “natural” does not mean they are not harmful or don’t have their own side effects. There are specialists who study the available evidence about integrative oncology, and it’s important to let your providers know if you’re using complementary and integrative therapies while you’re in treatment.
For most people, treatment will eventually end. It is estimated that more than 3.5 million people are alive right now who have been through breast cancer treatment, and most of these people experience ongoing impacts on their body, their finances, and their psyche.
People with metastatic breast cancer may be in treatment for the rest of their lives. Many live for years and may change treatment multiple times. Even for people with advanced cancers, there may be periods of remission when there’s no evidence of active disease.
The period immediately after treatment can be especially difficult. Many of the physical and psychological impacts of treatment do not end on the last day of treatment. It is not uncommon for someone to experience a surge in anxiety that the cancer might return after active treatment has ended. Some people who didn’t previously have a support group find it helpful after treatment. There are many resources for people after, as well as during, cancer treatment.
In acknowledgment of the ongoing impact of breast cancer on our lives and bodies, as well as the risk that our cancer may recur, many of us choose the phrase “living with breast cancer” instead of “survivor” to describe our relationship with breast cancer.
For free, one-on-one breast cancer information and resources, reach out:
• phone: 800/877.2.STOPBC
• email: info@bcaction.org
Disease and disability have a profound impact on our lives and our relationships. In addition to the person who is diagnosed—and has to go through treatment—cancer challenges our families, loved ones, and friends. And caregiving is both physically and emotionally demanding.
 It can be helpful to build a broad base of support that does not put too great a burden on any one person. No caregiver can do everything and caregivers will need to say no at times. It is important that caregivers are able to ask for and get help because caregivers also need support, whether they are stepping up for a short-term crisis or providing longer-term care. Caregivers will have their own feelings and physical needs that are just as valid as those of the person they are caring for. Depression is not uncommon for long-term caregivers, and there are resources to help.
It can be helpful to build a broad base of support that does not put too great a burden on any one person. No caregiver can do everything and caregivers will need to say no at times. It is important that caregivers are able to ask for and get help because caregivers also need support, whether they are stepping up for a short-term crisis or providing longer-term care. Caregivers will have their own feelings and physical needs that are just as valid as those of the person they are caring for. Depression is not uncommon for long-term caregivers, and there are resources to help.
Contact the Family Caregiver Alliance (caregiver.org) for more information or online support.
At Breast Cancer Action, we recognize that the personal is political. Breast cancer is a social justice issue and a public health crisis that impacts some communities disproportionately. It is a widespread women’s health crisis in a male-dominated and profit-driven society, and addressing and ending the breast cancer epidemic requires profound changes at every level of our society. Individual action alone, whether in terms of lifestyle or behavioral choices, is not sufficient to tackle the root causes of this breast cancer epidemic. We focus on systemic interventions that will address the root causes of the disease and produce broad public health benefits.
Breast Cancer Action was founded by women who met at a support retreat for women living with, and dying from, breast cancer. They discovered they shared a deep anger and outrage that more wasn’t being done to address the disease. And they decided to form a group and reach out to more women who shared their urgency to do something, both for themselves and for their daughters and granddaughters.
The outreach flier they developed from their first meeting in 1990 read: “We are meeting to organize Breast Cancer Action. Our goals are education and political action to prevent a further rise in the incidence of breast cancer; indeed, we hope that our efforts will serve in the future to lower the breast cancer rate in the United States.”
 Three decades after that first meeting, we carry on our founders’ fearless vision and commitment to education and political action. In order to address and end the breast cancer epidemic, we must tackle the root causes of these health inequalities, which are the result of a complex interplay of culture, power, economics, racism, and sexism. We believe that no single injustice can be effectively addressed in isolation, and we recognize that injustices in our society reinforce each other in many ways and at many levels.
Three decades after that first meeting, we carry on our founders’ fearless vision and commitment to education and political action. In order to address and end the breast cancer epidemic, we must tackle the root causes of these health inequalities, which are the result of a complex interplay of culture, power, economics, racism, and sexism. We believe that no single injustice can be effectively addressed in isolation, and we recognize that injustices in our society reinforce each other in many ways and at many levels.
Over the years we’ve accomplished a lot together, but we still have a long way to go. Both things are deeply true and drive our work every day here at BCAction. We hope you will join us in connecting your personal experience to larger systems and advocating for system change.
Visit BCAction.org to find out how to:
We are working for a world where lives and communities are not threatened by breast cancer. For as long as it takes, we will continue our work to achieve health justice for all women at risk of and living with breast cancer. We’re in this with you and for you, for the long run, and we know we’re stronger when we raise our voices together. Join us!
Most importantly, know we’re here for you right now—or whenever you need our help. Through our free Information and Resource service, we provide unbiased information about breast cancer to anyone who needs it. You can speak one-on-one with a knowledgeable staff member so you can make informed decisions. You can also access our vast resource of breast cancer information online at BCAction.org. Please contact us.
See What You Need to Know About Breast Cancer for essential, fact-based information for anyone who wants to learn about the disease.